The word vitamin is a relatively recent term. It first appeared in a dictionary in 1912 to describe organic substances in food, essential for most of the body’s chemical processes. Before vitamins were discovered, doctors recommended eating the right types of food: carrots (rich in vitamin A) to maintain vision, citrus fruits (rich in vitamin C) to prevent scurvy, and whole grains and vegetables (rich in vitamin B1) to prevent beriberi.
Essential vitamins
After years of research, 13 vitamins were identified as being essential for health. Essential because the body does not produce them and therefore they must be supplied by food and/or supplements. These essential vitamins are divided into two categories: fat-soluble and water-soluble.
Fat-soluble vitamins include vitamins A, D, E and K, which are stored in the body’s fat to be used when necessary. Given that the body stores fat-soluble vitamins, it is possible to ingest excessive doses of one or several of these vitamins, although this rarely happens. Too many vitamins can result in a number of symptoms, including headaches and irritability.
The essential water-soluble vitamins are C, B1, B2, B3, B5, B6, B12, folic acid and biotin. These vitamins are not stored in the body: the body uses the ones it requires for a specific function and excretes the rest through urine.
Many people think that if they take supplements, they won’t have to worry about following a balanced diet. But vitamins are just that: supplements. It is important to remember that one of the functions of the human body is precisely the absorption of vitamins through food. In addition, scientific research is constantly detecting supporting phytonutrients in foods that, along with vitamins, help maintain health and that are not available as a pill.
Another important point to remember is that an excess of certain types of vitamins may not be beneficial. While large amounts of some vitamins are helpful in some situations, an excessive amount can cause side effects that can be mildly disturbing (such as dry skin or sleep disturbances) or actually dangerous (such as liver damage).
How should vitamin supplements be taken?
- Take vitamin supplements with food to increase absorption. Fat-soluble vitamins should be taken with food that has some fat content.
- If you feel nauseous within half an hour of taking the vitamin, you might not have enough food in your stomach.
- Large doses should not be taken all at once. For optimal absorption, take several doses throughout the day.
Vitamin D
While vitamin D is not one of the most popular vitamins, it is one of the most important. It helps the body absorb and use calcium, and is essential for bone and teeth development. These are the characteristics of vitamin D that help prevent calcium deficiency diseases: osteoporosis and rickets (a disease that affects children and causes bow legs and knock knees). Indirectly, vitamin D stimulates nerve function, protects against muscle weakness, promotes normal muscle contractions, and helps regulate heart rate.
Vitamin D also promotes the proper functioning of the immune system, stimulating the thymus to produce immune system cells which, in turn, eliminate bacteria, viruses and other disease-causing microbes.
Despite its importance at so many levels, vitamin D is a relatively recent discovery. In the early 1930s, researchers isolated a substance from cod liver oil that would later be called vitamin D. Almost simultaneously, it was also discovered that when dehydrocholesterol (a cholesterol derivative found in the skin) was irradiated with ultraviolet light, it produced an identical substance. Given that vitamin D could be produced by the body when exposed to sunlight, it was nicknamed the sunshine vitamin. Even more interesting is that, although it is known as a vitamin, vitamin D actually acts like a hormone.
After the body ingests vitamin D through food or supplements, or is produced in the skin via sunlight, vitamin D travels to the liver and then to the kidneys where it is metabolised for the body to use. The vitamin that the body does not use is stored in fat cells.
How to optimise vitamin D levels
Vitamin D (25-hydroxyvitamin D [25(OH)D]) is a highly lipophilic molecule. When circulating in the blood, about 80% of the vitamin is bound to its carrier protein (vitamin D-binding protein [DBP]). Another 10% to 15% of vitamin D is transported by the transporter protein albumin. Only a minor part of vitamin D circulates freely in the blood, therefore providing greater availability to the cells.
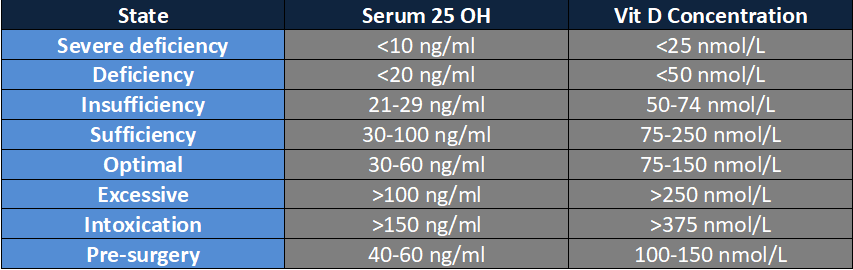
The serum concentration of 25(OH)D is the most reliable indicator for assessing vitamin D levels. However, measurement of 25(OH)D is technically quite difficult, due to its low concentration and the limitations of available test methods. Similar to other vitamins and blood components, vitamin D values are mainly expressed in nanomoles per litre (nmol/l) or in nanograms per millilitre (ng/ml), according to the unit system used: 1 nmol/l is equal to 0.4 ng/ml (conversion factor: 2.5). There are different discrepancies regarding vitamin D reference ranges, according to different recommendations. A level below 20 ng/ml defines deficiency. Optimal levels above 30 ng/ml are necessary to maximise bone health, among other vitamin D benefits. However, the most recommended range, considered adequate and healthy, is 40 to 60 ng/ml (100 to 150 nmol/l ). For individuals undergoing any type of dental procedure, values higher than 40 to 60 ng/ml are recommended, given that after a period of stress (such as a dental surgery), levels can decrease substantially.
Unfortunately, food does not contain high enough levels. Examples are cod liver oil (400–1,000 IU/tsp), fresh salmon (600–1,000 IU/3.5 oz vitamin D3), tuna (236 IU/3.5 oz vitamin D3), egg yolk (20 IU/vitamin D3 or D2) and milk, cheese or yogurt (100 IU/3 oz, usually vitamin D3).
According to the American Association of Clinical Endocrinologists (AACE) and the American College of Endocrinology (ACE) guidelines, supplementation is recommended to maintain levels above 30 ng/ml. The Endocrinology Society in the USA recommends reaching a concentration of more than 30 ng/ml (>75 nmol/L) of serum 25(OH)D, considering the ideal range of 40-60 ng/ml (100-150 nmol/L). The Endocrinology Society also advocates an intake of 1500-2000 IU/day (37.5-50 μg) in adults, considering that obese adult patients (BMI > 30kg/m2) should take three times the normal daily dose of the vitamin.
What are the recommended doses of vitamin D in the adult patient?
Over the years, different doses to increase the level of vitamin D and obtain a better state of health have been described in scientific literature. Many authors have recommended a higher daily dose than the corresponding authority guidelines. Most of these guidelines were focused on bone health. However, many studies have proven or suggested an important role for vitamin D in non-skeletal health. Based on the results, we suggest adequate daily supplementation rather than interval supplementation with a high dose. A clinical study showed that after increasing the vitamin D level to the required range, a daily dose of 2000 IU was insufficient to maintain the required vitamin D level for a longer time period.
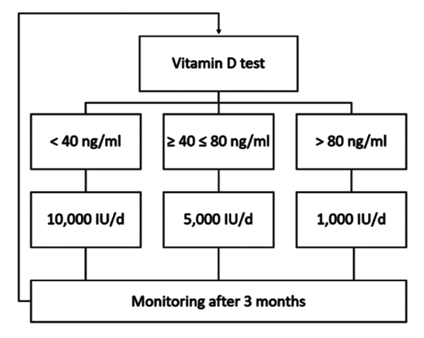
We recommend an individualised daily dose of vitamin D, according to the patient’s needs. A <40 ng/ml vitamin D level requires a daily intake of 10,000 IU to rapidly increase levels to 40-80 ng/ml. This dose has been carefully investigated and is shown to be safe. To maintain a healthy vitamin D level (40-80 ng/ml), we recommend a daily dose of 5000 IU. In cases where the recommended range of 40 and 80 ng/ml is exceeded, the daily intake of vitamin D should be reduced to 1000 IU. Studies reveal that the association of vitamin D3 with vitamin K2 can be beneficial for our body, since vitamin D3 ensures that calcium is easily absorbed and K2 (MK-7) activates the osteocalcin protein, responsible for integrating calcium in the bone. Finally, 25(OH)D should be monitored every 3 months to assess individual differences in vitamin D metabolism and allow further individual dose adjustments, according to patient needs.
The importance of vitamin D in dentistry
As already mentioned in the article published in “O Jornal Dentistry” together with Dr. Miguel Stanley and Prof. Doctor Shahram Ghanaati in 2020: “The importance of vitamin D in Dentistry: could it play a relevant role in the resistance of infectious diseases such as COVID-19?”, vitamin D plays a leading role in oral health.
Vitamin D plays an important role in supporting the immune system and in the integration of various biomaterials. It is also relevant for decreasing overall oxidative stress and minimising additional inflammation caused by surgery. Vitamin D is also involved in the integration of biomaterials and other metabolic processes, such as bone remodelling. For this reason, some complications have been related to vitamin D deficiency in the field of dentistry, such as the failure of dental implants and the integration of biomaterials due to vitamin D deficiency.
Vitamin D can also help prevent tooth decay as it strengthens tooth enamel. In addition, vitamin D can be considered a hormone that helps control periodontal disease, as it strengthens our immune system and helps fight chronic, infectious and inflammatory diseases.
For these reasons, the prescription of blood tests that include vitamin D should be advised to patients who are undergoing surgery, are susceptible to dental caries or have a periodontal disease, in order to contribute to the success of the treatments.




